When Livia Knipp’s water broke just 19 weeks into her pregnancy, the situation seemed very grim. The family from Windsor Heights turned their attention east toward Iowa City and UI Stead Family Children’s Hospital. The UI high-risk obstetricians and neonatal specialists gave the Knipp family a new beginning.
Story: Molly Rossiter
Videography: University of Iowa Health Care Marketing and Communications
Published: Dec 18, 2019
First birthdays are something to celebrate, so March 14, 2019, was a milestone for Kerigan Knipp, known as the “miracle baby” to her older siblings, Romey and Henrik. It’s a hard-earned nickname, one that evolved as Livia and Jason Knipp traveled a road from helplessness to hope, and ultimately back home with their young family.
On Feb. 9, 2018, Livia Knipp of Windsor Heights, Iowa, was nearly halfway through her pregnancy with her third child. Anticipating a Fourth of July baby, she booked a newborn photo session and later that day went to lunch with friends.
She was back at the Des Moines mortgage office where she worked when her water broke.
“I knew the second it happened that something was seriously wrong,” she says.
Livia was concerned—and scared. She called her local hospital. A nurse she spoke with didn’t seem to believe her. Frustrated, Livia found an online discussion forum where women shared similar stories of the amniotic fluid sac surrounding the baby rupturing.
“I had time to Google what happens with a gush of water at 19 weeks—all the babies I’d read about had passed away,” she says. “I was holding back tears because I knew something was wrong.”
She drove to the emergency room of a local hospital. Her husband, Jason, met her there and they were given grim news: Livia would be admitted because the baby would likely be born that night and would not survive.
“They told me to start planning a funeral,” she remembers. “It seemed so surreal. The day started so normally, and suddenly I’m sitting in a hospital room being told I was supposed to plan my baby’s funeral.”
Livia was admitted to a local hospital with the expectation the baby would be delivered soon. If it happened that night, doctors told her, there was little they could do.
An additional concern: Livia began to bleed.
“A midwife came in to talk to us. When she left, I stood up and the bed was full of blood,” Livia recalls.
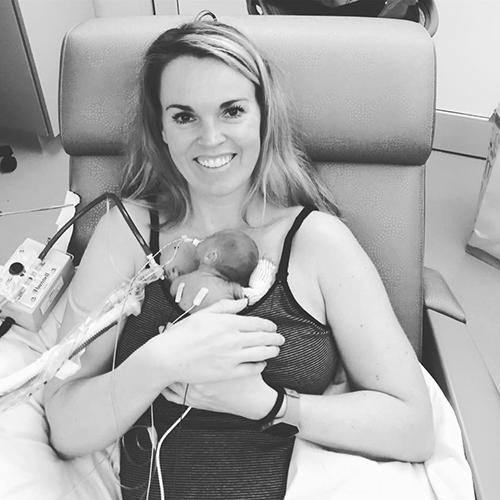
Kerigan Knipp was born by C-section on March 14, 2018, just 23 weeks and six days into the pregnancy. She weighed 1 pound 6 ounces—about the size of a liter of water. Her parents, Livia and Jason, gave her a middle name they had grown to love: Hope. “I just got that feeling from the moment we arrived at UI Hospitals & Clinics that everything was going to be OK,” Livia says.
The midwife returned and told Livia and Jason the baby would likely be born that night.
“That night we went to bed and I bawled all night,” Livia says.
Livia didn’t go into labor and was released from the hospital two days later with little hope that her situation would improve. Unless she remained pregnant until her 24th week—a milestone many hospitals use to determine viability—there was nothing they could do, doctors told her.
Even if the baby survived, local doctors said there was a greater chance for physical and mental disabilities, which is the case for most babies born after PPROM, or preterm premature rupture of membranes, the condition when the amniotic sac breaks before week 37 of pregnancy.
“We saw another doctor, and he said there was really no hope,” Livia says. “They told us to just let nature take its course and they’d have hospice calling in a few days. We left devastated.”
‘Get to the University of Iowa’
She took to social media to ask for prayers for the baby who wasn’t expected to survive. Her prayers were more than answered when a friend responded with news of a woman in Clear Lake, Iowa, who had experienced the same situation two years prior. That woman’s son was born at 23 weeks—and was doing well.
“This woman called and said, ‘You have to get to the University of Iowa,’” Livia says. “She started telling me everything about how the doctors there saved her baby, along the same timeline. It just sounded amazing and so much better than the ‘no hope’ we had been getting.”
The woman on the other end of the phone was Carrie Tysdahl, whose son Knox was born in March 2017 at 23 weeks and four days gestation. Knox spent four months in the Neonatal Intensive Care Unit (NICU) at University of Iowa Stead Family Children’s Hospital. Like Livia, Carrie’s water broke early, and local doctors told her there was nothing they could do. Knox went home in July 2017 after having had no major surgeries or procedures while in the hospital, despite his early start.
‘We have hope for you’
Livia went back to the internet and found this: At UI Stead Family Children’s Hospital, the survival rate for infants born at 22 weeks was 59%.
“We have a 0% chance staying here where they’re literally just going to hand us our baby and let it pass away in our arms, or a 59% chance just two hours away. We had to know we did everything we could to save our baby,” Livia says.

Helping Clear Lake boy beat the odds
Knox Tysdahl was born at 23 weeks gestation, or 17 weeks early, at Stead Family Children’s Hospital in 2017. UI Health Care’s large team of high-risk obstetricians, its Level 4 neonatal intensive care unit, and the attitude that every baby in its care will go on to live a healthy life helped ensure Knox would be another “micro preemie” success story.
In addition to the early rupture of her amniotic sac, Livia says, she continued to bleed heavily at home.
She told her doctor to transfer her care to UI Hospitals & Clinics. Sarah Wernimont, MD, PhD, a fellow in maternal-fetal medicine at UI Hospitals & Clinics, was the first physician assigned to her case.
The maternal-fetal medicine team specializes in high-risk pregnancies, whether the mother had complications going into pregnancy, developed complications during the pregnancy, or is having problems based on how the baby is growing inside the uterus.
“We have options that other places just don’t have, and part of that is related to our fantastic NICU doctors; they take care of a lot of babies born really early, and they push the envelope in terms of providing care to these babies,” Wernimont says. “As maternal-fetal medicine providers, we’re often in the hospital caring for these women as they’re trying to buy every single day they can of their pregnancy. We get to see firsthand how closely families work with the NICU doctors and how incredibly difficult it is to be in the hospital at this stage.”
For Livia, this was the answer she’d been looking for.
“I told Dr. Wernimont a little bit of my story, and she said, ‘We have hope for you,’” Livia says. “We hadn’t heard anything remotely close to that. No one had any hope for us up to that point.”
In consultation with Livia by telephone, Wernimont sent her to her local hospital for antenatal steroid injections to accelerate development of the baby’s organs. If she maintained the pregnancy to 22 weeks, she would be admitted at UI Hospitals & Clinics, where doctors would continue to monitor her and her baby.
“As soon as I got the shots, someone drove me to Iowa City. I wanted to be close in case I needed them sooner,” Livia says.
Livia’s pregnancy hit the 22-week mark on March 1, and she was admitted to the hospital. An ultrasound showed she had placenta previa, a situation where the placenta is low in the uterus and covers the cervix. Because the condition could lead to heavy bleeding if she labored, Livia was monitored closely, and the decision was made to deliver by C-section if her condition changed.
Livia stayed pregnant for 13 more days; Kerigan Knipp was born by C-section on March 14, 2018, just 23 weeks and six days into the pregnancy. She weighed 1 pound 6 ounces—about the size of a liter of water. Her parents gave her a middle name they had grown to love: Hope.
“I just got that feeling from the moment we arrived at UI Hospitals & Clinics that everything was going to be OK,” Livia says.
Happy endings
As medical director of the NICU at UI Stead Family Children’s Hospital, Jonathan Klein, MD, has cared for hundreds of premature and extremely premature infants. Each case is different, he says, but one thing is constant: there are obstacles between birth and going home.
The neonatal team at UI Stead Family Children’s Hospital is one of just a handful across the country that will perform life-sustaining efforts—such as monitoring the baby’s heart and lungs for signs of distress—for babies born as early as 22 weeks. The hospital’s survival rate for infants born at 22 weeks is about 59%, Klein says. He credits a fine-tuned formula based on collaboration and the belief that “premature birth isn’t a cause of death.”
“The most difficult thing initially, with a baby born this early, is making the acute, abrupt transition from fetal to neonatal life,” he says.
Babies like Kerigan need the nourishment they would normally get within the uterus but when born this early, it’s delivered through a nasogastric tube—a soft, thin tube passed through the baby’s nose, down the back of the throat, and into the stomach.
Lung development also is key, Klein says, and extremely premature babies start with a lung “plan” with the use of high-frequency ventilation, a process that allows them to breathe on a respirator in a way that doesn’t damage the lungs. The antenatal steroids Livia received helped Kerigan’s lungs develop enough to use the respirator.
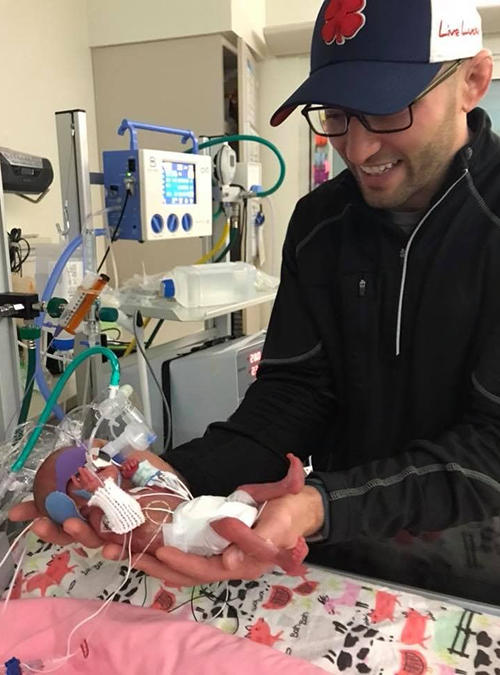
Jason Knipp holds his daughter Kerigan in the Neonatal Intensive Care Unit at University of Iowa Stead Family Children’s Hospital. Kerigan was born just 23 weeks and six days into the pregnancy.
“We have a culture that is very open to input from all the caretakers, not just the other physicians caring for these babies,” Klein says. “We work as a team, and we work with each other collaboratively, but we’re also very open to taking observations from the hundreds of brains that interact with this baby, including nurses, lab technicians, respiratory therapists, and the parents. All of that data streaming in allows us to have very good outcomes.”
Livia says Kerigan faced some scary moments during the four months they were in the NICU, including a diagnosis of pulmonary hypertension—a condition in which the blood leaving the right side of the heart faces increased resistance, or pressure, in the lungs—when she was 2 weeks old. Premature infants are at risk for pulmonary hypertension, but it didn’t stop Kerigan from going home on oxygen just a few weeks after her projected due date. She had been in the NICU for 135 days. She was on oxygen at home for a little more than a year but has been breathing on her own since April 2019. She has no other health concerns related to her prematurity.
For Klein, these stories never get tiring.
“When I see these babies in the clinic [after they go home], their weight is almost 10 times what it was at birth because they were so small. It’s hard to believe you can be normal and perfect when you start out that immature, with organs that aren’t designed to survive outside of the mom that early,” Klein explains.
“It takes a huge team dedicated to all of these subsystems to allow these babies to survive. I know the survival rate we have is quite high and the outcomes are quite good, but I’m always blown away that this is actually happening, that this is reality and it’s not a movie.”
