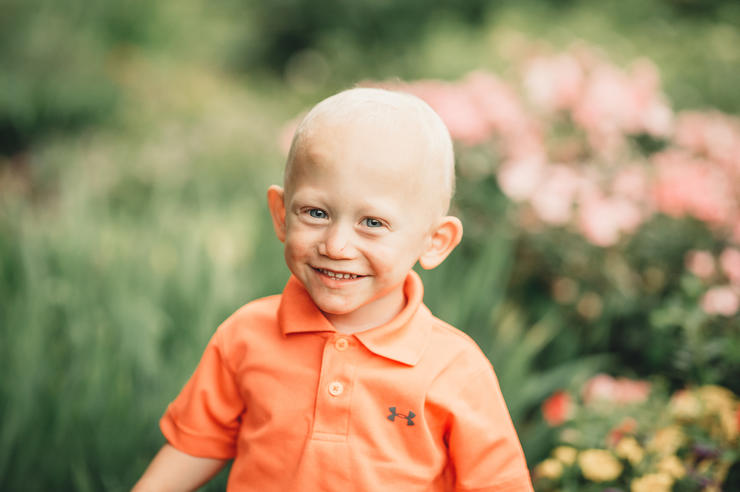
An easier way to monitor high-risk pediatric cardiology patients at home

Bringing a new baby home can be stressful for any parents but when Halle and Ethan Howard finally brought their son Charlie home, that stress was intensified. Charlie was born with hypoplastic left heart syndrome, a condition in which the side of the heart that pumps blood to the body is severely underdeveloped. Charlie had heart surgery four days after birth and spent the first two months in the hospital. The Howards, who now reside in Springville, Iowa, were finally able to bring him home in June, but he was still fragile and required close monitoring.
Fortunately, they had extra help with a new home monitoring program pilot project that allows families of pediatric cardiology patients to more easily document important patient information and share it with their care team in real time.
University of Iowa Stead Family Children’s Hospital is the first hospital in Iowa to introduce the home monitoring device, which consists of a specially programmed digital tablet that families use to record weight, oxygen levels, food intake and output, heart rate, medications, and any concerns. This data is accessed by the care team, who can identify potential health issues using the data. This new program makes communication between families and the care team easier, faster, more consistent, and improves at-home care for these vulnerable children.
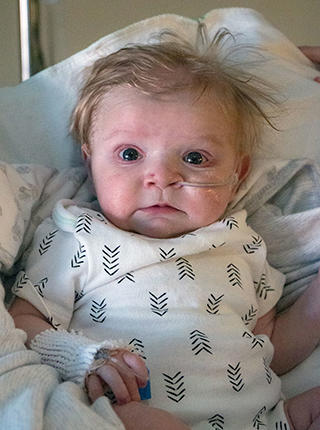
Charlie Howard was born with hypoplastic left heart syndrome, a condition in which the side of the heart that pumps blood to the body is severely underdeveloped. Charlie had heart surgery four days after birth and spent the first two months at UI Stead Family Children’s Hospital.
Family and care team connections available around the clock
“Our family was fortunate to be one of the first to use the home monitoring system. This new innovation allowed us to stay in contact with Charlie’s nurses and doctors 24 hours a day,” says Halle. “We were able to work with the care team from our home and determine if Charlie needs to go back to the hospital for immediate medical attention. They made it so easy for us to feel comfortable at home while giving our son the best possible care we can. We are never completely alone in this journey.”
Trudy Pierick, ARNP, is a pediatric cardiology nurse practitioner who was the pediatric single ventricle program coordinator and the Howard family’s main point of contact while they were caring for Charlie at home. She saw firsthand how this new program improves data collection for the family and streamlines communication between the family and care team.
“Because these infants are medically fragile, care at home can be time-consuming and intense. The parents have little free time, and gauging when to best contact them is a challenge. With the home monitoring system, I could access their data several times per day, look at trends, and see alerts for data that falls outside of our recommended parameters,” explains Pierick. “This allowed me to get a quick snapshot of how they were doing, with the option for more detail if needed. If there were questions or concerns, I followed up with the parents via phone call or text.”
Charlie’s parents used the tablet to keep track of his vital information. They have used it to research the difference between what is regular spitting up and vomiting, and track that data as well. During a review of Charlie’s information, Pierick saw something that concerned her.
“Trudy noticed a trend with Charlie’s vomiting and weight loss and encouraged us to come in to the hospital,” explained Halle.
Fast, consistent data sharing
Because the tablet helps ensure clear, consistent information can be seen by the care team, it relieved the Howards of having to explain Charlie’s case each time they spoke with a new person.
The single ventricle clinic at University of Iowa Stead Family Children’s Hospital is part of the National Pediatric Cardiology Quality Improvement Collaborative. This is a group of more than 50 pediatric cardiac centers across the country. The purpose is to improve care for children with complex congenital heart disease.
“Since the data was available for everyone on the care team to see, they were always up to date and we didn’t have to tell the same story over and over,” says Halle.
Before this program was introduced, families of infants with shunt-dependent heart disease like Charlie would document all this information at home on a paper worksheet in a binder.
“Previously, families tracked information in the binder, notified us via phone with concerns, and brought the information to clinic visits. The tablets allow information to be collected in real time, and can be viewed by care providers at any point, with alert notifications for sensitive issues,” says Pierick.
New parents have a lot to manage under the best of circumstances, and parents of high-risk infants have even more. Halle believes the new program helped them keep better track of all the details important to Charlie’s care at home.
“The tablet showed us baseline information for what we should expect in terms of wet diapers and stools. It has notifications for feedings. If we had to use a paper system, we might not be as accurate,” she says.
Personal contact between families and care teams has always been a top priority. This new program enhances that communication, creates a significantly better tool for data collection, and changes the way UI Stead Family Children’s Hospital provides outpatient care for this high-risk group of cardiac infants.